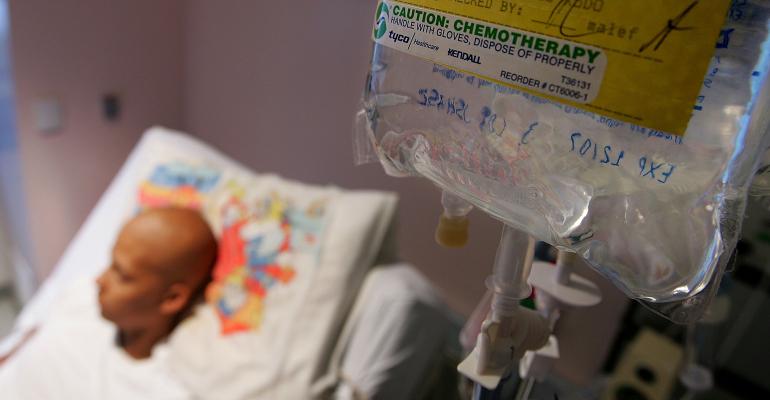
The stats are significant. According to the National Cancer Institute, one in three women and one in two men will receive a cancer diagnosis in their lifetime. That means no professional advisor can avoid dealing with the impact of cancer on clients and their families and loved ones.
While dealing with the more technical ramifications of such a diagnosis is essential to the role professional advisors serve (for example, legal documents to assure financial matters can be addressed during a period of illness, financial modeling to incorporate care costs, etc.), the threshold issue in advising your clients and families who just received a cancer diagnosis is navigating the tumultuous emotional waters they now find themselves in. Unless you can show the necessary empathy and ask the right questions, you may fail to fulfill your role in providing the expertise and technical guidance clients need.
When a client is in crisis following a cancer diagnosis, you have to take control, be direct in what information you need and guide the next steps. Clients with a cancer diagnosis, and their family members, don’t know what they need.
Case Study: Young Adult Diagnosed With Cancer
A young woman was 25 when she was diagnosed with cancer. Her mom took time off work to take her to the endless oncology and other medical appointments; her dad kept working. Fear, strain and pressure on the family grew as medical bills piled up, and a second income wasn't coming in anymore. This upper-middle class family had multiple homes, and there’s a possibility they were asset rich but cash poor. The 25-year-old graduated from grad school and was in the process of launching herself into the professional world when everything began to fall apart. She felt a tremendous amount of guilt over her perception that she was ruining her parents’ future and that they were spending tremendous sums of money on her care. She was also dealing with the fear of not even knowing if she would live through the cancer treatments and what she would do next if she even survived this. She went from being an independent adult in the working world to moving back with her parents for help and care. It was a dramatic change for the entire family. There was also a lot of fighting in their home, mostly about money and their respective futures. Many things changed for her family very quickly as a result of the cancer. The daughter’s optimistic hopes for a bright future dimmed. The parents’ dreams for their daughter, and plans for their retirement, all shattered instantly.
Case Study Questions
- How can you step into the maelstrom as an advisor?
- How can you guide this family to address their new financial, retirement and estate planning realities?
- What do you do now that the adult child is diagnosed with cancer (or any mental or physical health challenge)?
- How do you ask the questions of the family that you need to know to guide them? How do you find the right words?
- How do you prepare yourself to better handle these situations? Might it be advisable to incorporate key health-related questions into every client intake so that these become second nature? What about using role play with other colleagues to practice asking the questions that make you uncomfortable so that when you meet with client families in crisis you’ve already grown comfortable asking the uncomfortable questions?
Family Impact
Medical advances in treatments have improved dramatically for many types of cancers. In fact, improvements are so marked in some cancers that they’re viewed as a chronic illness as opposed to a terminal illness. The improved survival rates (especially with early detection), can have a tremendous impact on both the individual with cancer, the entire family and your role as an advisor. So, you need to understand:
- What diagnosis does the patient/client have? Is it terminal, and if so, what’s the anticipated survival period projected for the client? If it’s not terminal, how can you project and plan for a longer life expectancy for the client (for example, you don’t want to underestimate life expectancy and thereby incorrectly project future financial needs)? See https://curesearch.org/What-Does-the-Literature-Say
- What’s the prognosis? How will it affect the client: physically, mentally, emotionally, occupationally and financially?
- How will current treatments affect the client? Will treatments impact cognitive abilities, making it more difficult to plan? Might that necessitate involving other family members or friends in the process? Do you have, or can you get, the legal authorization to work with those designated? Will the medical treatments so impact cognition that the client may not be able to sign legal documents so that the process should be accelerated?
- How much care will be required? For how long? Who will provide that care? Will they be paid or family/friends? Will others who contributed to finances have to cut back on work? How will all of this impact financial planning for the family in their new reality? The loss of even half of an income might make the family’s financial status precarious.
Family members may not know how to deal with the diagnosis and all that it potentially holds for their future. They may feel a lot of pressure to carry the load of the entire family and be uncertain about everything that may come next in the present, and in the future, they imagined for themselves and their family. They may avoid discussions, appear unreasonably optimistic (or unreasonably pessimistic), spend more time working, drinking or escaping into other areas of their lives. Everyone deals with this trauma differently. If you can identify any of these reactions, it will better equip you to help the family and offer outside resources to help them cope.
Consider planning to provide financial resources for the care and help of not just the patient but also the caregiver or other family members. Too often, the only focus is on the patient, but the entire family will be impacted. If the caregiver isn’t provided for, whether that means respite time, counseling, therapy or other needs, that caretaker may burn out and not provide optimal care. It may also so strain the relationship and result in the potential of the caregiver abandoning the patient/client (for example, through divorce).
Establishing Roles
Everything can change and likely will. The nature of the changes will depend on the age of the person diagnosed. If you can be attuned to these variations, it may help you anticipate the impact and better advise the client. If the individual is a child, and there are other children in the home, who will take the other children to their activities and spend time with them while the child diagnosed is getting treatment or needs extra caretaking when they’re feeling especially sick? If a parent must stay home, or a financial provider is the one diagnosed, where will the financial resources come from to sustain the family? This is why understanding the diagnosis is vital to providing the financial support that’s within your expertise. If the period of care is anticipated to be limited and the child is anticipated to recover, different planning may be feasible than if the situation is anticipated to require years.
If it’s a parent of adult children, are there siblings who can help even if they’re not local? Does someone new need to be hired, or does another extended family member need to be brought in temporarily to help with all the responsibilities? Who will be the point person on interacting with the medical team? What might this cost? Who and how might it be paid for? What will insurance cover? Discussing and defining these roles immediately will alleviate a lot of stress, confusion and chaos.
Creating Boundaries
The client can and should create boundaries. Your client is an individual with her own responsibilities, feelings and limits. It’s OK for the client to say “no” to people who may be overbearing in their effort to help, or demanding in their efforts to spend time with your client. It’s OK for the client to limit things that feel extra, for example, taking on a new project at work, agreeing to volunteer at the PTA bake sale, etc.), and hand off responsibilities or activities she’s in charge of currently.
As an advisor, if you become aware of boundary issues from comments the client or family members make, you should encourage the family to involve a counselor. If the family has a counselor, you should ask for the counselor to participate to some degree in the planning process or perhaps that you be given authorization to confer with the counselor. Your obtaining that type of professional input may equip you to better guide the family as to financial, legal or other matters you’re focused on.
It’s also important to understand your own boundaries. Your clients may feel comfortable sharing intimate details of their lives with you for hours on end. It’s OK for you to place limits on the time you’re able to spend with them, be honest about not having expertise as a mental health counselor or oncologist, and provide referrals to professionals who are experts in the other areas where they need support.
One empathic way of doing this is to use phrases like “I know you’re struggling right now, and this can’t be easy. I’m an expert in the financial or legal elements of planning, but I’m not an expert in how to navigate the emotional and other areas where families need support after someone is diagnosed with cancer. I would like to be able to provide you with a list of resources you can call next week and follow up with you to make sure you got the support you need. I know you have a lot on your plate and it’s easy for tasks to fall to the wayside. Can I get your permission to follow up by phone or email on Tuesday of next week if I haven’t heard back from you yet?”
Seeking Support
After a client receives a diagnosis, all parties will likely feel anxiety, sadness, anger and uncertainty about what their lives will look like moving forward. Getting support is essential to coping in a healthier way. Some resources your client may consider are friends, other relatives, mental health professionals and support groups. Although the client may feel guilt around hiring someone, it’s OK for her to hire someone because she may not have the physical, mental or emotional capacity to take on everything.
If this occurs, you need to be alert to possible issues of undue influence. Who’s the individual helping? Will that individual benefit from the process? Is there any risk or evidence of overreaching? In the opposite situations, if it becomes apparent that the client is overwhelmed, consider suggesting: “You’re one person and can’t do it all. It’s OK to get help.” You might even demonstrate that it is affordable for them to do so, as the financial considerations of further help may be a source of angst to the client.
Advisors should remember when a client is struggling to cope with the myriad new challenges cancer brings, she’s likely cognitively overwhelmed. Thus, repeating advice given may be necessary. Providing simple bullet lists of follow-up items after a meeting or call may be essential to help keep the client focused. Keeping client “to-do” lists to perhaps three or four prioritized items may be more effective than long memorandums. When items on that initial client “to-do” list are checked off, an updated list may be provided. Consider using web-based meetings in lieu of phone calls or in-person meetings. A web meeting with a video camera, more than just a phone call, may give you a much better sense of how a client is actually faring, as well as her reactions to points you make. Be sensitive to the fact that the client might not want a web meeting due to discomfort over how they look, etc. Following the meeting, call or web meeting, set a time to follow up so that the client will have a date and time to add to her calendar that will keep the process moving.
Communicate
As explained above, communications with both the patient and other family members will be affected by the emotional impact of a cancer diagnosis. Communications with the patient may also be affected, at varying degrees and at different times, due to the cognitive impact of the disease, pain medications or treatments. Be mindful of this. Be certain to ask questions to assess the current status. Don’t assume that if your last conversation was clear or not, that the next conversation will be the same way. Be mindful that all individuals involved may be agitated, tired, stressed and unable to process information as they did before the diagnosis. So plan shorter communications. Even if your typical client practice is to have a two-hour comprehensive meeting to address all issues, that approach may not work for the patient and family dealing with cancer. Shorter, more-focused meetings and communications may be more digestible.
Advisors’ Role
Patients having received a cancer diagnosis, along with their family and loved ones, need the help and guidance of their professional advisors. That advice may be more important than ever before. However, to be effective as an advisor, you need to be sensitive to the changes, and subsequent impact, that the diagnosis, treatment, emotional reactions, and changes in family and other interpersonal relationships have on the patient and their family members. Keep in mind that patients and clients don’t know “what they don’t know.” Ask a lot of questions. Do not be uncomfortable asking difficult questions. That’s your role and the key to providing the very services and advice that makes you an expert.
Amanda Koplin, LPC, is the CEO of Koplin Consulting LLC, a national concierge mental and behavioral health company. Martin M. Shenkman, Esq. is an estate planner in Fort Lee, N.J.